Persistent seasonal outbreaks of Lassa fever have continued to ravage Nigeria 52 years after it was discovered in the country. This has resulted in a loss of lives among the general public and health workers.
The recurrent outbreaks of cholera also leave in their wake attendant health and socio-economic consequences.
- Nigeria loses as Russia-Ukraine war escalates global oil prices
- Police arrest pastor over shooting of teenage girl
Medical experts say several factors account for the persistent outbreaks of the two diseases in the country.
They say the country has been majorly reactive in its response to epidemics, and not doing enough to prevent them.
They also say members of the public and the government have critical roles to play to ensure that Nigeria does not continue to witness the outbreaks.
Burden of the two diseases
According to the Nigeria Centre for Disease Control (NCDC), since the beginning of this year, the Lassa fever outbreak has claimed 59 lives with 358 confirmed cases of the disease recorded in 19 states, and 65 local government areas.
In January alone, Nigeria recorded 40 deaths from Lassa fever representing a case fatality rate (CFR) of 19.0 per cent.
In the sixth epidemiological week of this year, seven new healthcare workers were infected with Lassa fever in Bauchi, Ondo and Edo states.
In January, three doctors were killed by the disease in Nasarawa State.
Also, cholera claimed 3, 604 lives in 33 states and the Federal Capital Territory (FCT) in 2021, the NCDC said.

Over 50 people died in July 2021.
The centre in its situation report said a total of 111,062 suspected cases of the disease were recorded across the states within the period.
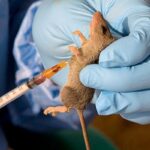
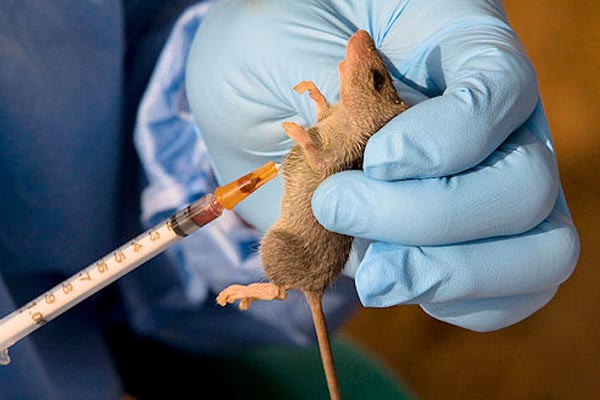
Lassa fever is a viral haemorrhagic illness, caused by contact with food or household items contaminated with rodent urine or faeces.
The virus is carried in multimammate rats, the common soft-furred African rat whose female has a double row of breasts.
They normally live in bushes and visit nearby homes for food, which they contaminate. The virus has an incubation period of 6-21 days.
The Lassa virus may also be spread between humans through direct contact with blood, urine, faeces, or other bodily secretions of a person infected with Lassa fever, laboratory transmission can also occur.
The illness is characterized by sudden onset of fever, and general weakness. Other symptoms include headache, sore throat, muscle pain, chest pain, nausea, vomiting, diarrhoea, cough, and abdominal pain may follow. In the most severe cases, individuals may bleed from the mouth, nose, eyes or other parts of the body and eventually die.
Sometimes, a large percentage of Lassa fever cases may be unnoticed because it has similar symptoms to other common diseases.
While more cases of the diseases occur during the dry season, it occurs all year-round.
Cholera is a disease of the intestinal system caused by a bacteria called Vibrio cholera. It is usually transmitted through the faeco oral route which means ‘from faeces to mouth’ or from hands contaminated with the bacteria put in the mouth.
“Once the bacterial is transmitted from either food, water or any other sources contaminated with the bacteria into the mouth, it then has the propensity of igniting the disease process in the individual,” Dr Dawal Kwande Solomon, a Consultant Family Physician said.
While there are numerous causes of vomiting and diarrhoea, in the case of cholera, the frequency of the passage of the watery stool is actually quite significant.
Reasons the diseases persist
Dr Emmanuel Alhassan, Nigeria Coordinator, Global Health Advocacy Incubator (GHAI) which funds the Prevent Epidemics project, said one of the major reasons the two epidemics persist is because efforts and funding in the country are more channelled towards responding to the outbreaks than preventing them.
He said, “You know, rather than spend less money to put structures in place to prevent, we are always reacting and it costs much higher to react after something has happened. So, it is a huge challenge.
“For instance, the NCDC is supposed to get a percentage of the Basic Healthcare Provision Fund (BHCPF), now we hear that they are in the process of trying to do the guidelines.
“It will be a shame if at the end of the day they say that money should be used for responding to outbreaks rather than for prevention. The money is not all that much, so it is better to use that money to prevent epidemics.”

Alhassan said “the NCDC should also use that money to ensure it strengthens prevention in
areas affected by Lassa fever and cholera; because just like COVID-19, it is better, more sustainable, easier, and less expensive to prevent than to react.”
Dr Akor Godday, a family medicine physician, said the outbreaks persist because the populace are not doing enough in protecting themselves against the disease.
Asked if the government was doing enough in preventing outbreaks of the two diseases, Dr Godday said while the government has its roles to play, the public has a more crucial role to play in preventing the diseases.
He said, “like Lassa fever for example, it is not the government that sends rats to people’s houses. It is people who create dirt in their houses, and refuse to close or cover their food items such as garri and rice.
“When they allow pieces of food around, and an infected rat that has Lassa fever enters the house, and either defecates or urinate upon the food items and they cook it or just take it like garri, they will come down with the infection. And because they live in the same house with others, the disease will continue to spread from one house to another.
“I think the first thing we should look at in this case is if the individuals that have the houses are ensuring optimal care because if all food items in the house are well covered after preparation, and then there is no dirt and waste bin within the house, definitely a rat that is infected with Lassa fever will not come into the house, and as long as they don’t have access into the house, individuals there will not come down with the infection.”
The expert said the situation also obtains with cholera.
“So, if an individual or people living in a community decide to be defecating close to the river or close to ponds instead of having a toilet facility, when it rains and this person doesn’t wash his or her hands and decides to touch another water or have a hand shake with another person, or even prepare food with those contaminated hands, as many people that come in contact or eat the same food with him will definitely come down with the infection.”
Dr Godday said while cholera case is a disease that has to do with inadequate water supply or poor personal hygiene, in communities where the government is not able to provide water, if the people ensure that they have toilets, even pit latrines that enable their waste to be disposed of properly, they will not come down with cholera.
“However, we know that the masses are entitled to water supply and basic amenities so we don’t want to say we will not call on the government.
“The government has roles to play in providing water, however, even when it makes the water available and the masses don’t follow the basic rules of washing hands, and avoiding passing stool in water bodies, among others definitely the disease will continue to ravage the country,” he added.
Prof Idris Mohammed is a professor of medicine and immunology, and a past Chief Medical Director of the University of Maiduguri Teaching Hospital (UMTH) said despite 60 years of trial, Nigeria’s effort at developing emergency preparedness and response mechanism has failed and to date, there is no proper emergency preparedness and response in place to address epidemics of pandemics that occur without notice.
“That is the truth of the matter, but with the establishment of the Nigeria Centre for Disease Control (NCDC) and also with greater awareness that has been brought about by COVID-19, people are now appreciating the need for emergency preparedness and response and I hope that we move forward from then on and make progress,” he added.
On vaccines for Lassa fever not developed till date, Prof Mohammed said, “But the problem with vaccines development, first of all, is that pharmaceutical companies need to spend a minimum of $150 million for one vaccine, and that is for a cheap one, and yet you may not even succeed.
“So, with Lassa fever, it is not easy for companies to handle sending samples from patients from West Africa to Europe to use the serum to extract the antigens against which they will prepare the vaccine. It is time and money-consuming as well. So, there are many reasons why the vaccines have not been developed.”

How individuals, health workers can prevent Lassa fever, cholera
For Lassa fever, NCDC advised Nigerians to eliminate rats in their homes and communities using rat traps, block all holes in their houses to prevent entry of rats, and also avoid touching rats with their bare hands.
The organisation added that hand hygiene is one of the most effective ways to reduce the spread of infectious diseases like Lassa fever.
“Encourage the practice of regular hand hygiene among family and friends to stay healthy.
“Store foodstuff like rice, garri, beans, corn/maize, etc in containers that are well covered with tight-fitting lids. Avoid drying foodstuffs outside on the floor, roadside where they will be exposed to contamination.
“Avoid bush burning which can lead to the displacement of rats from bushes to human dwellings,” NCDC advised.
Dr Ogugua Osi-Ogbu, a chief consultant physician and in charge of Lassa fever infection control at the National Hospital, Abuja, advised health workers to maintain a high index of suspicion, standard procedures and hand washing when managing patients.
She also enjoined family members of any victim of the disease to take precaution while attending to their infected relations through avoiding direct body contact with the patients’ fluid, through the use of gloves and also taking the patients to the hospital as soon as sign of ailment is seen.
Dr Dawal Kwande Solomon said a person taking dirty water and being where there is a cholera outbreak is at high risk of being infected either from food, water, or any other contaminated sources.
He said people can protect themselves from getting the disease through personal hygiene and environmental hygiene.
He said maintaining personal hygiene means that “you should always wash your hand with soap and water or where there is no soap, use ash.”
He said environmental hygiene involves clearing away dirty water and making sure the water that one consumes is treated through boiling or using chlorinated solutions before ingesting, in order to kill the bacteria in the water.
He also advised people taking care of anyone presenting with diarrhea and vomiting to wash their hands very well whenever they come in contact with the person’s clothing and faeces.
Dr Solomon said government has an important role to play in terms of general community water supply and providing some of the agents for people to treat the water they use, especially during an outbreak.
NCDC ‘s response to outbreaks
NCDC said the agency has activated the National Lassa fever multi-partner, multi sectoral Emergency Coordination Centre (EOC) to coordinate response activities at all levels.
The Director General of the agency, Dr Ifedayo Adetifa, said “This became necessary given the increase in the number of confirmed Lassa fever cases across the country and a joint risk assessment with partners and sister agencies.”
He said since 2016, NCDC has worked hard to improve diagnostic capacity for the disease.
“Currently, seven laboratories can conduct confirmatory tests for Lassa fever in Nigeria and are coordinated by the NCDC National Reference Laboratory (NRL). This has improved active case detection for the disease.
“In addition, Nigeria through NCDC is participating in the largest-ever Lassa fever study that aims to provide an accurate assessment of the incidence of the disease in West Africa. This will also accelerate the development of vaccines and therapeutics for Lassa fever,” he added.
For cholera, NCDC said the response is being coordinated by the national multi-sectoral technical working group hosted at NCDC in collaboration with the federal ministries of health, water resources health, Federal Ministry of water resources and partners.
It also provides onsite/offsite support to states and surveillance in all states among others.
The agency said it has also been carrying out senistization programmes about infectious diseases for the citizenry and health workers.
 Join Daily Trust WhatsApp Community For Quick Access To News and Happenings Around You.
Join Daily Trust WhatsApp Community For Quick Access To News and Happenings Around You.